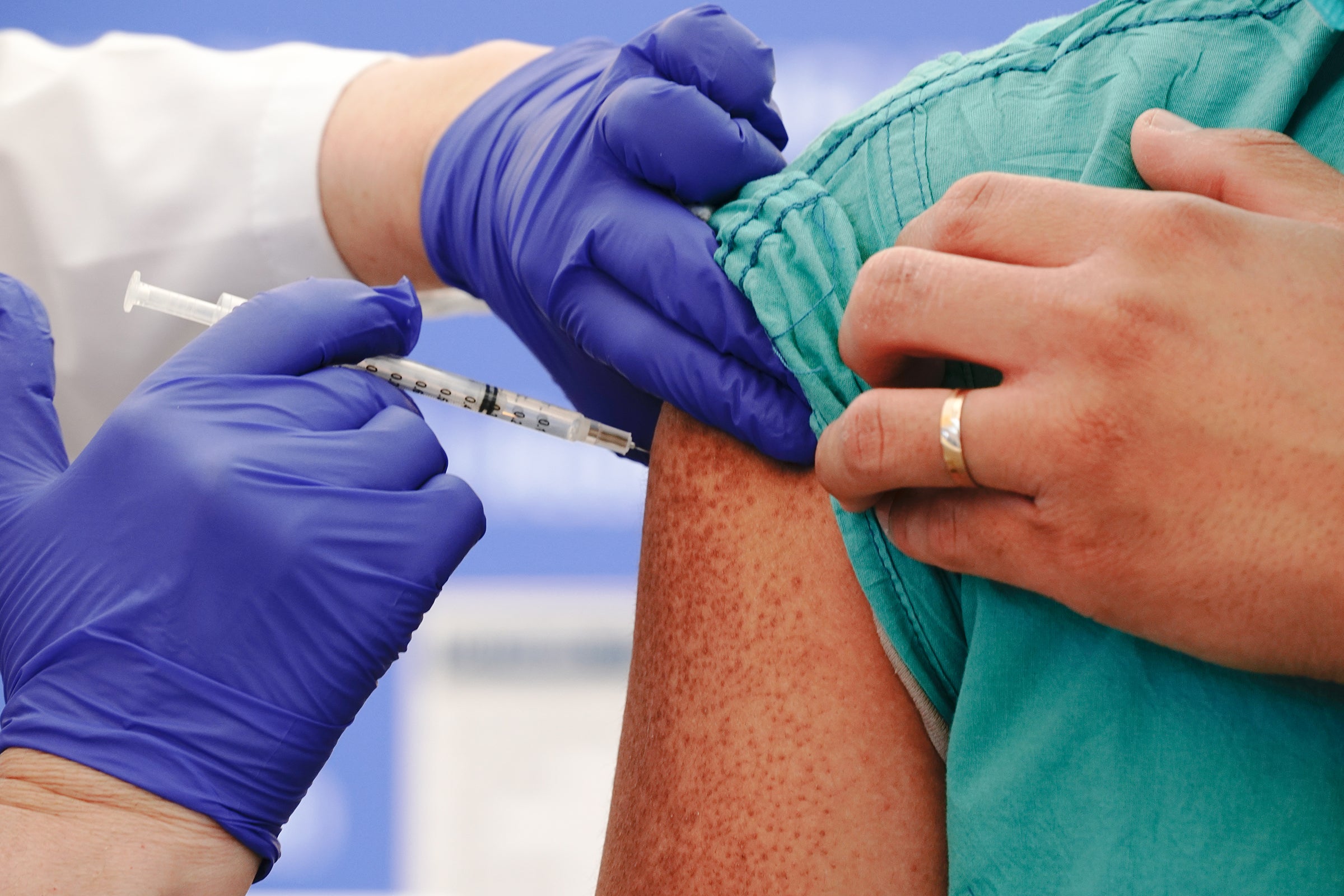
The Omicron-driven COVID surge has caused considerable upheaval during this pandemic winter. Despite the availability and efficacy of COVID vaccines, many people with a history of suspected allergies to the first mRNA COVID vaccine dose—reactions such as hives, swelling, shortness of breath and/or low blood pressure—have not gotten their full series.
Their fear is understandable. After all, the U.S. Centers for Disease Control and Prevention currently states that there are two contraindications to the COVID vaccine: “severe allergic reaction (e.g., anaphylaxis) after a previous dose or to a component of the COVID-19 vaccine,” and “known diagnosed allergy to a component of the COVID-19 vaccine.”
Yet as an allergist/immunologist who has been seeing such patients on a daily basis for the past year, I believe that the CDC is wrong and should change its guidelines. Based on my experience and others’, in most cases, people with prior allergic reactions can safely receive both mRNA COVID vaccine doses, as well as the booster. And my colleagues and I have developed a protocol that allows us to deliver them.
A true severe allergic reaction to the COVID vaccine is exceedingly rare, on the order of two to five per million people inoculated. What’s more, billions of people have now received the COVID vaccine, and as far as we know, no one has died from an allergic reaction. The CDC should update its guidelines, to assuage the fear of people who are concerned that a second allergic reaction to the vaccine will send them to the emergency room, or worse. This clarification would not only reassure patients of the vaccines’ safety, but also prevent people from fraudulently claiming newly discovered vaccine allergies as a reason to demand exemptions from employer and government mandates.
In December 2020, as vaccines were first authorized for use, and people were alarmed about reports of allergic reactions, a couple of things were immediately clear: For unknown reasons, allergic reactions occurred more often in women, yet people with a history of food, venom and medication allergies could safely receive the vaccine. They just needed to be monitored longer than people who had no history of allergies after their injections.
After the vaccines became widely available in the spring, the medical community was still in the dark about what was causing the allergic reactions. One possible culprit was an IgE-mediated reaction to polyethylene glycol (PEG), a common ingredient in bowel preps, pharmaceutical preparations and cosmetics, and also a component of both mRNA COVID vaccines. PEG maintains the stability of the solid lipid nanoparticles encasing the mRNA.
My colleagues and I began skin testing for allergies to PEG, as well as the COVID vaccine itself, focusing on people who had had a probable allergic reaction to their first dose of the COVID vaccine. Our experience with PEG testing, however, was mixed: people who tested positive for PEG allergies were, in nearly 40 cases, still able to successfully receive both doses of the vaccine.
That PEG might not be the allergenic culprit was borne out in a study that looked at 80 patients who had allergic reactions after the first dose of an mRNA COVID vaccine. Regardless of their PEG skin test results, most of these people could safely be given the second dose. Another study evaluated 105 people who had reactions to the first dose of the mRNA COVID vaccine, and 85 percent of these patients received the second dose without problems. Among the remaining 15 percent were people who declined further vaccination or opted instead for the Johnson and Johnson vaccine. These studies, while small, do challenge the assumption that PEG is responsible for these adverse vaccine reactions.
Given the limits of PEG skin testing, we developed a vaccination protocol in line with what vaccine allergy experts recommend. If a person has a suspected anaphylactic reaction to the first COVID vaccine dose, we first determine if the reaction was truly allergic via a skin test. Other conditions, such as anxiety attacks or vasovagal reactions, which involve a sudden drop in blood pressure and heart rate after a stressful trigger, can be mistaken for anaphylaxis.
If skin testing for allergies to COVID vaccines is negative, we give the next dose in the clinic, with at least 30 minutes of monitoring afterwards. In the rare instance where skin testing is positive, we divide the vaccine into smaller volumes, and administer them in quick succession over an hour, until the patient gets the full dose.
With this protocol, I have been able to administer the COVID vaccine, whether the first, second, or booster dose, to every patient I have seen, regardless of prior allergic history or testing results. So if NFL quarterback Aaron Rodgers, who misleadingly said he was “immunized,” then claimed an unspecified allergy to a COVID-vaccine component, had come to my office, our protocol would have likely allowed him to be vaccinated.
In the meantime, we are still trying to understand what causes a COVID vaccine allergy in the first place. One possibility is that the linking of PEG to nanoparticles activates part of the allergy-response side of the immune system. Another possibility is that the solid lipid nanoparticles themselves interact with the syringes used for injections, creating something allergenic.
Whatever the cause, physicians are using placebo-controlled clinical trials to confirm what has become well-documented in the medical literature. One NIH clinical trial is evaluating the safety of the COVID vaccine in people who’ve had a history of severe allergic reactions from any cause, such as medications and foods. Another NIH clinical trial is looking at the safety of giving the second COVID vaccine to people who’ve had systemic reactions to the first dose. Of course, the CDC shouldn’t wait for the results of these trials before removing the contraindications to getting the COVID vaccine, as the benefit of getting the vaccines clearly outweighs the minuscule risk of allergic reactions.
More than one year after the introduction of COVID vaccines, the share of people fully vaccinated in the U.S. sits at an abysmal 63 percent. The CDC must update its COVID vaccine allergy advice to accurately reflect allergists’ experiences on the ground, especially with Omicron’s fierce transmissibility. As someone who rarely steps into the hospital, I have largely stayed in the background the past two years of the pandemic, while my colleagues have been shouldering the brunt of the responsibility in the hospital. Now, with the ability to safely vaccinate almost everyone with a history of severe allergies, whether to a vaccine component or the vaccine itself, this protocol is how I can do my part to help end the pandemic.
